Premier Philadelphia Academic Medical Center Implements Masimo Wearable, Wireless Patient Position, Orientation, and Activity Sensors in its ICUs
Masimo and Temple Health today announced that Temple University Hospital (TUH), a 722-bed academic medical center located in Philadelphia, is expanding its use of Masimo technologies with Centroid, a wireless patient position, orientation, activity, and respiration rate sensor, at 100 beds across its ICU units.
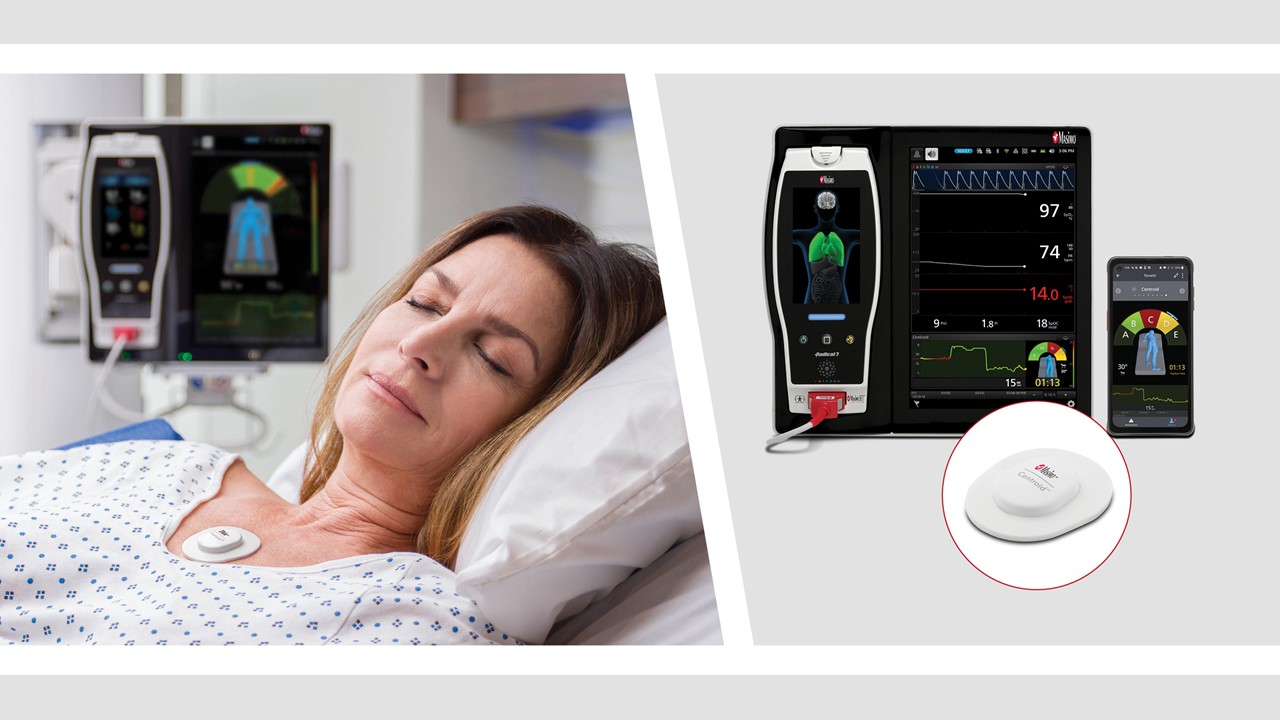
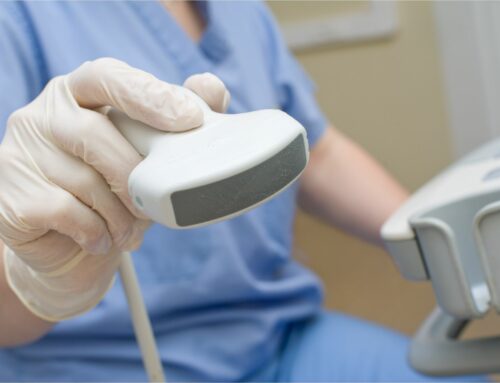
According to Masimo, Centroid helps clinicians monitor patient position to avoid preventable pressure injuries, and can alert clinicians to sudden movements such as fall-like events. In addition, Centroid detects chest movements to continuously provide respiration rate, assisting clinicians with additional data that may inform care decisions. Centroid pairs with the Root Patient Monitoring and Connectivity Platform using Bluetooth to track a patient’s posture, orientation, and activity, providing the ability to monitor patient position and detect changes in position. The data transmitted by Centroid can be displayed in various formats on Root, giving clinicians multiple ways to assess adherence to protocols regarding tissue stress and to tailor care to the specific needs of each patient. In addition, Centroid data can be relayed via the Masimo Hospital Automation platform to Patient SafetyNet, Masimo’s centralized remote patient supplemental monitoring platform, and Replica, a mobile application that allows clinicians to view continuous data regardless of location.
At TUH, all ICU beds are being equipped with Root and with Centroid, including the Trauma ICU, Cardiothoracic ICU, Burn ICU, Neurological ICU, and Medical Respiratory ICU. Angelo Venditti, DNP, RN, Executive Vice President for Patient Care and Chief Nursing Executive at Temple Health, said, “We are pleased to expand our relationship with Masimo, which has already proven itself as a key technology partner in our efforts to improve patient outcomes. When we trialed Centroid, we found it helped our teams prioritize workflows more effectively, with increased focus on following turn protocols and decreased incidence of pressure injuries.”
Hospital-acquired pressure injuries (HAPI), commonly known as bed sores, are on the rise – occurring in nearly 5% of all hospitalized patients in the US.1 Elderly and critically ill patients are often at highest risk for developing a HAPI, which can lead to further treatments and extended lengths of stay in the hospital.
To compound the patient impact associated with these pressure injuries, there is a major economic burden for the hospital as well. Pressure injuries are classified as a “Hospital Acquired Condition”, or HAC, and the treatment costs associated with HACs are non-reimbursable to the hospital. One pressure injury can quickly add up to tens of thousands of dollars. Many facilities in the US spend millions each year treating these wounds.2 Pressure injuries are also a reportable quality metric to CMS.3
According to the National Pressure Injury Advisory Panel (NPIAP), scheduled turning protocols are known to prevent HAPIs, yet most hospitals in the US still use techniques such as paper wall clocks or egg timers to try and optimize this practice4 – methods that are proving to be ineffective and archaic in modern healthcare. Staffing issues and competing priorities have strained nurses across the US, and staying on top of when a patient was last turned is difficult without a more sophisticated system.
Centroid is a single-patient-use adhesive sensor indicated for the orientation monitoring of patients who may be susceptible to pressure ulcers by tracking patient movement and activity using an accelerometer and gyroscope. Centroid can identify a patient’s position and orientation to the nearest degree, with alerts based on the duration in a static position to help clinicians adhere to hospital patient turn protocols. Centroid also features customizable alarm zones to help avoid patient positions that could negatively impact recovery time. Unlike simple time-based rotation protocols, Centroid provides an advanced pressure risk algorithm that takes into account the cumulative pressure exposure time, with body segment-by-segment resolution, using the integrated gyroscope, displayed on the Root screen using color-coded markers. This can help clinicians not only identify if a patient has been turned, but also identify if the new position may still be resulting in pressure risk to the same tissue—and ultimately, helping to guide clinical decisions about the most appropriate, least risky positions for each patient.
Temple Health and Masimo have been pulse oximetry technology partners since 2008. Temple implemented Masimo Patient SafetyNet in 2014, has since expanded their Patient SafetyNet system to seven units, and has also adopted Masimo SpHb noninvasive hemoglobin monitoring, NomoLine capnography, SedLine brain function monitoring, O3 regional oximetry, and now the Centroid patient positioning tracker.
Joe Kiani, Founder and CEO of Masimo, said, “We are honored to continue to be able to equip Temple—one of the country’s premier medical institutions—with so many of our life-saving solutions, from monitoring technologies like SET pulse oximetry and rainbow Pulse CO-Oximetry, to advanced monitors like Root and Hospital Automation solutions like Patient SafetyNet. With the addition of Centroid, Temple adds another key Masimo innovation to their toolkit. It’s a great example of our commitment to developing new ways to provide the highest quality, most relevant data to clinicians in the most intuitive, useful formats. We look forward to helping Centroid prevent many HAPIs and improve the outcomes and lives of their patients.”
About Masimo
Masimo is a global medical technology company that develops and produces a wide array of industry-leading monitoring technologies, including innovative measurements, sensors, patient monitors, and automation and connectivity solutions. Our mission is to improve patient outcomes, reduce the cost of care, and take noninvasive monitoring to new sites and applications. Masimo SET Measure-through Motion and Low Perfusion™ pulse oximetry, introduced in 1995, has been shown in over 100 independent and objective studies to outperform other pulse oximetry technologies.5 Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,6 improve CCHD screening in newborns,7 and, when used for continuous monitoring with Masimo Patient SafetyNet™ in post-surgical wards, reduce rapid response team activations, ICU transfers, and costs.8-11 Masimo SET is estimated to be used on more than 200 million patients in leading hospitals and other healthcare settings around the world,12 and is the primary pulse oximetry at 9 of the top 10 hospitals as ranked in the 2021-22 U.S. News and World Report Best Hospitals Honor Roll.13 Masimo continues to refine SET and in 2018, announced that SpO2 accuracy on RD SET sensors during conditions of motion has been significantly improved, providing clinicians with even greater confidence that the SpO2 values they rely on accurately reflect a patient’s physiological status. In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC™), carboxyhemoglobin (SpCO), methemoglobin (SpMet), Pleth Variability Index (PVi), RPVi™ (rainbow PVi), and Oxygen Reserve Index (ORi™). In 2013, Masimo introduced the Root Patient Monitoring and Connectivity Platform, built from the ground up to be as flexible and expandable as possible to facilitate the addition of other Masimo and third-party monitoring technologies; key Masimo additions include Next Generation SedLine Brain Function Monitoring, O3 Regional Oximetry, and ISA™ Capnography with NomoLine sampling lines. Masimo’s family of continuous and spot-check monitoring Pulse CO-Oximeters includes devices designed for use in a variety of clinical and non-clinical scenarios, including tetherless, wearable technology, such as Radius-7 and Radius PPG™, portable devices like Rad-67, fingertip pulse oximeters like MightySat Rx, and devices available for use both in the hospital and at home, such as Rad-97. Masimo hospital automation and connectivity solutions are centered around the Masimo Hospital Automation™ platform, and include Iris Gateway, iSirona™, Patient SafetyNet, Replica™, Halo ION™, UniView, UniView :60™, and Masimo SafetyNet™. Additional information about Masimo and its products may be found at www.masimo.com. Published clinical studies on Masimo products can be found at www.masimo.com/evidence/featured-studies/feature/.
ORi and RPVi have not received FDA 510(k) clearance and are not available for sale in the United States. The use of the trademark Patient SafetyNet is under license from University HealthSystem Consortium.
References
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3217823
- https://www.cms.gov/Medicare/Quality-Initiatives-Patient-Assessment-Instruments/Value-Based-Programs/HAC/Hospital-Acquired-Conditions
- https://pubmed.ncbi.nlm.nih.gov/30693644/
- https://cdn.ymaws.com/npiap.com/resource/resmgr/white_papers/1i._pressure_ulcers_in_indiv.pdf
- Published clinical studies on pulse oximetry and the benefits of Masimo SET can be found on our website at http://www.masimo.com. Comparative studies include independent and objective studies which are comprised of abstracts presented at scientific meetings and peer-reviewed journal articles.
- Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
- de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;Jan 8;338.
- Taenzer A et al. Impact of pulse oximetry surveillance on rescue events and intensive care unit transfers: a before-and-after concurrence study. Anesthesiology. 2010:112(2):282-287.
- Taenzer A et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
- McGrath S et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
- McGrath S et al. Inpatient Respiratory Arrest Associated With Sedative and Analgesic Medications: Impact of Continuous Monitoring on Patient Mortality and Severe Morbidity. J Patient Saf. 2020 14 Mar. DOI: 10.1097/PTS.0000000000000696.
- Estimate: Masimo data on file.
- http://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.
About Temple University Hospital
Temple University Hospital’s mission is to provide access to the highest quality of health care in both the community and academic settings. The 722-bed academic medical center supports Temple University and its Health Sciences Center’s academic programs by providing the clinical environment and service to support the highest quality teaching and training programs for health care students and professionals, and to support the highest quality research programs. The hospital’s values are simple: Respect, Service and Quality. Temple University Hospital – Main Campus (TUH) is a nationally respected academic medical center that offers high-quality care, the latest technology and skilled staff – all on a safe, easy-to-reach campus. As the chief clinical training site for the Lewis Katz School of Medicine at Temple University, TUH is a teaching hospital where the latest procedures and techniques are pioneered and where students and other physicians come to learn. It is also a robust research center that is advancing the fight against disease, pushing the boundaries of medical science and altering the course of serious disease. All of this means that Temple physicians and staff are at the forefront of medical knowledge. TUH is many things to many kinds of patients. For some, it’s the hospital they depend on for their routine medical care. For others, it’s a place to receive specialized, lifesaving treatments that can’t be found at most hospitals. Temple’s nationally renowned medical staff offer dozens of powerful new options for patients who, just a few years ago, were considered untreatable. So whether a patient needs a family doctor or a highly trained specialist, chances are good they can find that physician at Temple. Although surrounded by modern equipment and state-of-the-art facilities, it’s notable that Temple physicians and staff never lose sight of what is most important – patients and their families. This personalized approach to care makes the hospital a true medical home for hundreds of thousands of patients each year.