By Eliott Jones, CEO and co-founder at Biospectal |
Technology has changed medicine for the better. Doctor appointments are more likely to be held these days via Zoom chat than in an office. Vital data about your health like blood pressure and oxygen saturation can be gathered just as easily at home as it can in a medical office. Medical data is also no longer stored in a file and thrown in a cabinet; it is collected using an app and provides a constant, evolving picture of a patient’s health. The COVID-19 pandemic forced people to embrace these changes since in-person health care was limited to only critical needs. The thrust of the pandemic coupled with changes already in motion demonstrate virtual medicine is working. It not only enables better access to care; it provides smarter and more efficient allocation of medical resources as well.
The number of changes in the medical field in the past 18 months is staggering. On a larger scale, vaccines were created and millions of Americans inoculated in record time. However, changes are being most widely seen at the local level. For starters, more clinics and hospitals closed as telemedicine became the preferred model. Yet, the adoption of telemedicine also created job opportunities and even led the largest legacy healthcare providers to embrace and accelerate adoption of new technology. Even the way doctor offices are run has changed: both doctor and patient need to mask up and patients often have to wait outside, although some of those changes are loosening with increased vaccinations.
The 6Ps of Medicine
All of these changes toward a patient-specific, technology driven care model are part of 5P Medicine: Preventive, Predictive, Participatory, Personalized and Pertinent. The move toward telehealth during the pandemic accelerated these shifts on a massive scale, adding a sixth “P” to the mix: platforms. The “6P” model is driven by robust data and the opportunity to harness it through new connected technologies. It gives medical professionals a view of a patient’s overall health and allows for customized care and improved outcomes that are optimized for the patient. You’d never get a holistic personal snapshot of a health condition or disease with the customary 15-minute doctor’s office visit. With more information and better tools to make it meaningful in the clinical regimen, doctors can use those 15 minutes to review data and determine the best treatment. Time is better spent on what matters most and provides the best use of expert, and expensive, resources: collectively working on a plan for a patient to achieve optimal health.
Here’s how the six P’s of medicine work — and why they are improving healthcare and ultimately leading to better long-term health.
Personalized
Many of us grew up visiting a doctor who took a nearly identical approach for each patient. “Cookie cutter” medical care benefits no one, however. The Body Mass Index (BMI) that suggested ideal body weight based on gender and height has been discredited because it doesn’t account for healthy tissue or muscle mass. It simply makes no sense to evaluate the health of a bodybuilder the same as you would evaluate an obese person who weighs the same amount.
Available technology now allows doctors to better understand each patient’s health and put together a road map to vitality by accumulating a volume of data that is unique to each patient: blood pressure, average heart rates, blood sugars, oxygen saturation and more. Doctors will be able to view a patient’s overall health not just once, but over the course of many years. The end result is a comprehensive look at a patient’s health rather than the often inaccurate snapshot you get in a single office visit. Think about what a doctor could do with patient data that has accurate readings and vital signs. Why settle for one chapter of a book when you can now have the whole volume?
Precision
Patients have been able to remotely monitor vitals like blood pressure and blood sugar for decades. But the tools used – particularly those used to monitor glucose – were not always accurate or intuitive. In 2021 we’ve progressed far beyond simple blood pressure cuffs or glucose strips. The tools available can track all elements of your health, including alarm signs for a COVID -19 infection. Here are just a few advancements: A monitoring system can measure a woman’s luteinizing hormone and progesterone. The BioIntelliSense BioButton is a disposable device that sticks to your upper chest and allows healthcare providers to monitor vital signs to screen for COVID-19. The advancement of technology means many types of devices are as accurate as those used in hospitals and healthcare facilities.
Predictive
Health care crises can come out of the blue. That said, consistent monitoring can prevent many things from becoming issues in the first place. If you are diabetic, you can use a continuous glucose monitor to show fluctuations in blood sugar not only day-to-day or week-to-week, but minute-to-minute. Using this information, doctors can make informed predictions about where the patient’s blood sugar readings will be in a few months and adjust medication and care.
Preventive
It’s a universal truth: the more we know, the better informed we are to make decisions. When doctors have years of data about a patient’s health or a chronic condition, they can recommend interventions, change medications, or enlist other specialists if needed. An informed view of what could happen in the future could lead patients to make changes where they matter most: the present. If you know cholesterol is an issue for you thanks to preventative medicine, you can make positive changes like embracing vigorous exercise and switching to a healthy diet.
Patient Participatory Medicine
The idea of consumers monitoring their health is not new. “White coat syndrome” — a condition where blood pressure spikes due to nerves in a medical setting — has led patients to purchase portable blood pressure cuffs to monitor their blood pressure measurements at home. The advent of new devices, apps, and platforms allows patients to participate much more in their own healthcare. The new distributed model of healthcare fundamentally shifts from something static — “my doctor tells me what to do once or twice a year” — to a model where each patient is a stakeholder and a collaborator in their care. Active investment in an individual’s health leads to better outcomes across the board.
Platform
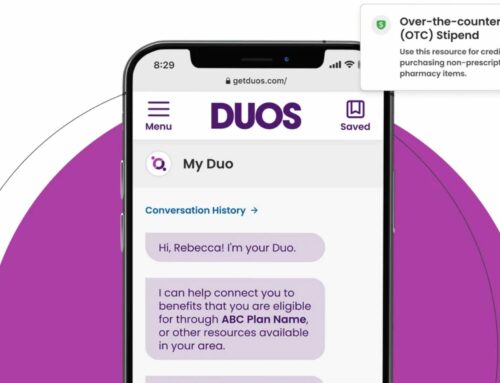
Distributed, cloud-connected health monitoring technologies add a sixth “P” by combining robust data into a platform that underpins the care regimen. Devices like smartwatches and other wearable sensors have helped people participate in their own healthcare and fitness for years, albeit in a limited way until now. Apps today are even better as cloud connectivity and maturing medical record and patient management systems enables near frictionless democratization of access to health monitoring by enabling instant, global scale distribution to existing smartphones and data integration with clinical patient management protocols. Almost everyone is equipped with a smartphone, meaning the platform for these technologies is ubiquitous if the health monitoring technology is software delivered via an app.
My company, Biospectal, turns the camera lens of a smartphone into a highly accurate optical blood pressure measurement and monitoring device that allows for discreet readings anytime, anywhere. The readings are particularly accurate because they can be taken without the customary bells and whistles that often lead to transient blood pressure increases. Other companies are also stepping up. QuardioArm is a wireless blood pressure monitor that syncs with your Apple Watch. The FibriCheck app monitors heart rhythms and can detect arrhythmias. Google’s Fit tracking platform uses a Pixel phone camera to measure heart and respiratory rate and other benchmarks. These types of apps help track progress and promote daily use, and they can connect seamlessly with healthcare providers to support treatment outcomes that improve health, longevity and quality of life and lower cost of care.
The Possibilities Of New Health Care
Not everyone is on board with all of the changes taking place. Some critics think the embrace of technology will damage the doctor-patient relationship and leave the bulk of the work to devices. I am more optimistic about where we’re headed. It’s not going to be a dystopian future where patients are monitored only by devices and have little discussion or even interaction with the people making health care decisions. Instead, the “6 Ps” will improve doctors’ understanding of their patients’ condition by offering medical professionals access to data and vital parameters collected in the patient’s “real-life” setting. These collective changes will have a tremendous positive effect on the cost of healthcare, patient outcomes and doctor-patient relationships.
Look at the trends and it’s clear things are headed in the right direction. Patients will contribute to and be involved in their health in a way that hasn’t existed before because of real-time feedback. Doctor-patient communication will improve. Education, coaching and behavior management will be customized based on data and then packaged and delivered via smartphones. Ultimately, technology and platforms will allow patients to participate at the highest possible level in the management of their health.
Not all of these changes will be easy — particularly for people who grew up with the traditional model of healthcare and were accustomed to visiting a doctor in person even for small matters. That’s why it’s incumbent on us along with medical professionals to spell out the reasons why technology will make lives and medicine better. Instead of focusing on the technology, focus on the end result: shorter wait times, more accurate data, better understanding of our health and even less time in a doctor’s office. The “6Ps” offer a path not only to make health care sustainable, but also to ensure it best serves those who matter the most: patients.
About the Author
Eliott Jones is the CEO and co-founder of Biospectal. He is responsible for leading the company’s overall strategy, product vision, go-to-market planning and execution. A digital product innovation and medtech startup veteran, Eliott has worked in executive roles building digital innovation and driving strategy, digital product design and development for major brands, including Yahoo, Landor Associates/Young & Rubicam, Intuit, Logitech and Rambus. He holds a degree in Visual and Environmental Studies, Magna Cum Laude from Harvard University.