Brian Wodlinger, PhD
Exact Imaging (manufacturer of the ExactVu™ micro-ultrasound system)
Not long ago patients with an elevated PSA (prostate-specific antigen) score were faced with the unfortunate ordeal of a prostate biopsy. A large number of men continue to undergo this painful diagnostic procedure with little benefit and risk the very real possibility of a post-biopsy infection. Thankfully, over the past decade the situation has begun to improve with a variety of more specific tests available to help better inform patients on whether a biopsy may be reasonably postponed or avoided altogether.
Multi-parametric magnetic resonance imaging (mpMRI), in particular, has shown considerable promise to help men avoid a biopsy as well as improve biopsy outcomes. For this reason, the National Comprehensive Cancer Network (NCCN) now recommends physicians consider mpMRI prior to prostate biopsy (NCCN Clinical Practice Guidelines in Oncology V1.2019, 2019)[1]. Unfortunately, mpMRI has several drawbacks, including a longer and more complex care pathway, poor performance by radiologists who do not specialize in prostate cancer, increased cost, and use of gadolinium-based contrast agents[2]. Further, for some patients who have decreased kidney function, are claustrophobic or have a pacemaker, MRI may not be an option.
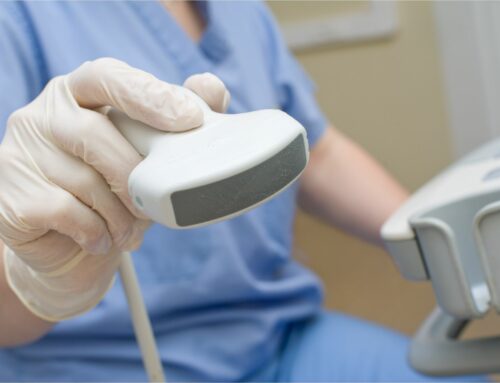
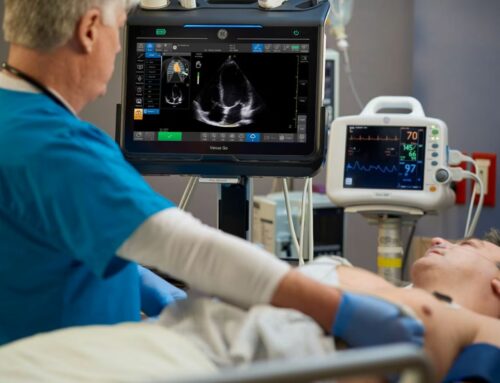
Micro-ultrasound is a new, improved ultrasound technology that operates at 29MHz and offers a dramatically higher resolution down to 70 microns, which is the thickness of a human hair, and the size of a typical prostatic duct. This higher resolution allows micro-ultrasound to detect prostate cancer with very high sensitivity, which was not possible using conventional ultrasound (Abouassaly, et al, 2019; Pavlovich et al., 2013)[3],[4].
What is particularly exciting about this technology is that it can be used just like regular ultrasound, in real-time by the physician performing the biopsy directly in the clinic. This speeds up screening, simplifies care, is less expensive, and does not require any contrast injections. The ability of micro-ultrasound to overcome the drawbacks of mpMRI is why the recently published study by Laurence Klotz, MD and colleagues, comparing mpMRI with micro-ultrasound, and published in the Canadian Urology Association Journal is so exciting (Klotz et al., 2020).[1]
The study reports on 1,040 men who received both mpMRI and micro-ultrasound imaging prior to biopsy. This large-scale, real-world study involved 11 institutions in the United States, Canada, and Europe, and world leaders in mpMRI. The goal was to compare the sensitivity and negative predictive value (NPV) of each imaging test to predict whether cancer would be found in a biopsy.
These are important metrics because they can help patients make an informed decision about whether or not to have a biopsy. In particular, NPV is the rate of finding only benign tissue in a biopsy following a negative or non-suspicious imaging result. The higher the NPV, the higher the patient’s confidence in avoiding a biopsy when the imaging is negative. In this study, micro-ultrasound demonstrated a higher NPV than mpMRI (85% vs. 77%, p=0.04). Micro-ultrasound also demonstrated a higher sensitivity (94% vs. 90%, p=0.03), which is the percentage of all cancers that were detected.
More importantly, these benefits were realized without any decrease in specificity or positive predictive value, suggesting both techniques would allow roughly the same number of men to avoid biopsy. For the average man in this study, a negative micro-ultrasound reduced the risk of finding cancer by 62%, while a negative MRI reduced the same risk by 41%.
What does this mean for patients? It may mean that instead of the urologist referring a patient out for mpMRI he can perform a micro-ultrasound scan in the office, which takes approximately 15 minutes. Together with other risk factors and biomarkers the results will help patients feel more confident in their decision to either proceed with a biopsy or to postpone it.
As with any clinical study, there are limitations to these results and further large-scale investigation is warranted. The authors note that due to the real-world nature of this registry there was no uniform biopsy protocol with patients at each site receiving differing numbers of biopsy samples. Further, many of the sites were not rigorously blinded to the MRI data leading to an important source of bias, however the authors state that “results between the blinded and unblinded sites were similar.” They conclude that micro-ultrasound is an appealing alternative to mpMRI for detecting prostate cancer.
Author Biography
Dr. Wodlinger is Vice President, Engineering and Clinical at Exact Imaging. Prior to Exact Imaging, Dr. Wodlinger held research positions at the University of Pittsburgh Medical Center and Case Western Reserve University. This research won Popular Mechanics Top Breakthroughs of the Year award and has been featured in the popular media on platforms such as CBS’s “60 Minutes”. He holds 8 patents in the medical devices space, has designed and executed more than 13 clinical trials and has authored more than 18 peer-reviewed research articles in prestigious journals such as The Lancet, and PLoS ONE. Dr. Wodlinger holds a PhD and MSc in Biomedical Engineering from Case Western Reserve University and BASc in Engineering Science from the University of Toronto.