by Dr Jarrel Seah, Medical AI Consultant at annalise.ai and radiologist registrar |
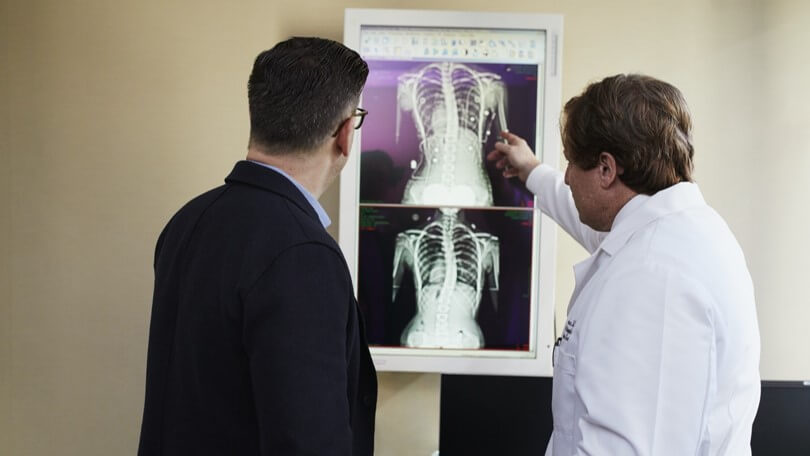 The humble chest radiograph is one of the most widely performed radiological examinations in the world and is capable of identifying abnormalities across a breadth of anatomical and physiological systems. With its wide availability and low radiation dose, it is used in developing and developed countries as a first-line imaging tool for assessment of the chest. (Schaefer-Prokop C, Neitzel U, Venema HW, Uffmann M, Prokop M. Digital chest radiography: an update on modern technology, dose containment and control of image quality. Eur Radiol 2008; 18: 1818–30., United Nations Scientific Committee on the Effects of Atomic Radiation. Sources and effects of ionising radiation, 2008.
The humble chest radiograph is one of the most widely performed radiological examinations in the world and is capable of identifying abnormalities across a breadth of anatomical and physiological systems. With its wide availability and low radiation dose, it is used in developing and developed countries as a first-line imaging tool for assessment of the chest. (Schaefer-Prokop C, Neitzel U, Venema HW, Uffmann M, Prokop M. Digital chest radiography: an update on modern technology, dose containment and control of image quality. Eur Radiol 2008; 18: 1818–30., United Nations Scientific Committee on the Effects of Atomic Radiation. Sources and effects of ionising radiation, 2008.
Over the years, chest radiography techniques have steadily improved, from film to computed radiography and subsequently digital radiography. These improved the standardisation, spatial resolution, contrast resolution, and accessibility of chest radiography. As a result, interpretation of chest radiography has become ever more complex, with more and more subtle pathology being identified. Similarly, the increasing accessibility of chest radiography means that its interpretation has evolved from a niche specialty skill in the early 20th century (https://pubmed.ncbi.nlm.nih.gov/1609679/) to a key clinical skill taught in medical schools. It is a skill that is now expected of almost every medical practitioner.
Despite its widespread use by and familiarity amongst medical practitioners, the chest X-ray interpretation remains challenging. While demonstrating excellent resolution, the chest radiograph is a flat projection of the complex three-dimensional structure of the chest and therefore, pathology is often partially obscured. As a result, critical pathologies such as lung cancer are often missed (White CS, Salis AI, Meyer CA. Missed lung cancer on chest radiography and computed tomography: imaging and medicolegal issues. J Thorac Imaging 1999; 14: 63–8.).
AI models hold great promise for being the next evolutionary step for chest radiographs. In particular, comprehensive AI models, defined as models that cover findings seen in the vast majority of studies, may bring about a new era of improved chest radiography. As the volume of chest radiographs performed continues to increase, comprehensive AI models (https://www.thelancet.com/journals/landig/article/PIIS2589-7500(21)00106-0/fulltext) may help medical practitioners rapidly and accurately identify not just acute findings but also key incidental findings such as lung cancers or bone lesions, ultimately leading to better patient care and improved health outcomes.
AI models have the potential to address the fundamental challenges facing medical imaging today. Comprehensive and consistent tools to assist interpretation promise to help identify all pathology and reduce errors. Faster interpretation times could help clear backlogs. Triage tools that identify patients likely to need urgent care promise to help make the best use of radiologist’s time in underserved systems. Anonymised stores of structured AI predictions promise novel capabilities in population health and other healthcare research. As the adoption of comprehensive AI models gradually increases, their beneficial effects on patient outcomes, clinician accuracy, and radiologist efficiency will grow and become an indispensable component of clinical practice.
 About the Author
About the Author
Dr. Jarrel Seah is a medical AI consultant at annalise.ai