By Nishant Panchal, CTO and Co-Founder at Noteworth
Digital transformation was already underway, but Covid-19 accelerated its adoption.
Can a massive dose of data actually make you better? It is a question that more and more healthcare providers are answering in the affirmative, although sometimes cautiously. Today, more than half the nation’s healthcare providers are using Big Data in one form or another, and even more are expected to follow.
But for anyone raised to understand the importance of accuracy and precision in so many areas of human activity, there is something about the concept of Big Data that seems deeply unsatisfactory. After all, how is Big Data really any different than noise? The influx of data doesn’t always translate to relevant or useful information.
The adoption of interconnected systems is causing the size of Big Data to constantly grow. Big Data in healthcare includes information from all types of sources including clinical health records, medical imaging, claims data, patient generated health data, public health data, data generated from academic studies, pharmaceutical data, and more. This makes it challenging to segregate and filter Big Data in forms where it can be digestible.
An estimated 80 percent of patient information remains unstructured making it more challenging to mine data. Taken in aggregate, that glut of information is both too large and too complex to be processed using traditional software applications. To combat this, innovative new forms of data processing, including some using artificial intelligence and machine learning, are being devised to make sense of it.
Yet there is more than enough already available in digital form to allow healthcare Big Data to be converted into clinically actionable information and, over time, to transform the entire industry. Until this year, the transformation of healthcare into a digital enterprise had been gradual and underway for the better part of a decade. Then, as COVID-19 peaked across the US, the need for remote and digital care delivery became a core tenant of healthcare.
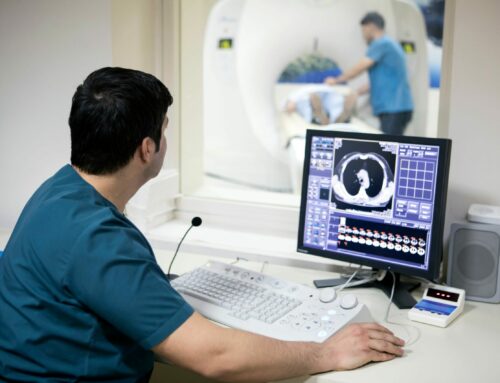
As a result, in the early spring of 2020, uses of telehealth and virtual care exploded to as much as ten times their pre-pandemic levels affecting essentially all areas of therapy. Telehealth services soon accounted for more than 40 percent of primary care visits for patients with traditional Medicare – up from one tenth of one percent before the pandemic struck. An Executive Order was signed calling on Congress to make telehealth a permanent fixture of Medicare. And public acceptance of the change has been tremendous.
In addition to providing a measure of relief to overworked healthcare professionals, virtual visits have been advantageous to homebound patients and to those in distant rural areas, for whom in-person office visits would be difficult or impossible. Using remote technologies as their vehicle for healthcare service delivery, caregivers can also collect current as well as past patient information, including data from digital devices that are either housed with or worn by the patient. Combined with other sources of Big Data, that information can then be contextualized and analyzed to provide personalized treatments.
Even in the field of mental health, online therapy sessions augmented with Big Data can be of real value. Using large external data sets, researchers can identify hard-to-recognize patterns in patients and identify risk factors for mental health including genetics, chronic health issues, stressors, and other factors that can help treat or even prevent the onset of mental illness3.
Applying the extensive body of knowledge represented by Big Data can improve diagnoses, accelerate treatments, enhance doctor-patient relationships, reduce errors, and in other ways upgrade healthcare. But its impact on patient care is only part of the story. Big Data also forms the foundation for a different, more meaningful financial model for the healthcare industry itself. Instead of reimbursements based on services, Big Data enables reimbursement to be based on value delivered to the patient. Providers can be graded on the quality of care they deliver as measured through an assortment of data sources.
However, the full benefits of Big Data in healthcare remain to be seen. That’s because a series of barriers to successfully implementing Big Data strategies remain to be overcome. These include a shortage of technical skills needed to analyze and manage a deluge of data, the cost of upgrading hospital and healthcare system architecture, measures to ensure the privacy of health information, compliance with complex regulations affecting personal data ownership and uses, and securing public trust in the institutions and technologies that are frequent targets of ransomware and other malicious attacks.
That said, however, Big Data has made huge inroads into essentially every sector of the economy. Examples include finance, telecommunications, and technology, all of which are major users of Big Data today. As a result, each of them is benefitting in practical as well as transformative ways. The healthcare ecosystem is only scratching the surface of the impact of Big Data. The coronavirus has greatly accelerated the volume of Big Data generation, and notwithstanding its somewhat hazy definition, Big Data will play a growing role in the digital transformation and application of healthcare delivery.