Mark Wehde with the Mayo Clinic was the keynote speaker at DesignCon, an engineering conference and expo in San Jose, where he discussed the future of healthcare. Afterward Mark agreed to a Q&A to dive deeper into the key points of his presentation.
We’re in the midst of a transformative era with regard to medical device innovation. What technologies are driving this innovation?
We’re moving into what is conventionally thought of as the fourth industrial revolution, and this is the digital platform revolution and there’s just a whole host of technologies that are coming together to allow us to solve problems in ways that we haven’t been able to before. And that includes some of the ones where we’re well aware of advances in genomics, which have been coming for 20 or 30 years. We sequenced the human genome back in the nineties and keep wondering, when is this going to have a real impact on the things that we’re doing? And we’ve gotten to the point where over the next decade, it’s going to be having significant impact. We see how quickly the RNA vaccines were developed for COVID.
And that was because of the power of some of this new technology, but we’re also going to see just huge impacts across all industries from AI and machine learning. Certainly, in healthcare where we’re seeing that other technologies, 3D printing is making huge inroads in the medical space because we’re now seeing that we have the ability to do point of care manufacturing of medical devices. And so that’s also very, very powerful, but I think really the big challenge or the big opportunities over the next decade are really in that digital platform space. So wireless technologies, remote monitoring you know, loud cloud-based data store, the ability to develop new algorithms for doing diagnosis and treatment, using the power of AI and machine learning. It’s really going to inform the way that we treat patients.
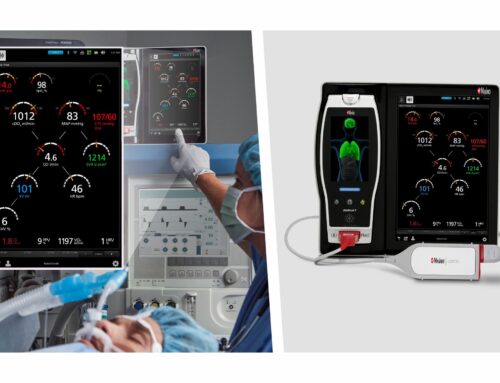
And we’re seeing that already today at Mayo clinic, we’re putting in a fairly robust AI factory. I’m doing that in partnership with Google. And our goal is to be able to take novel AI algorithms that are developed to figure out how to integrate them into the clinical workflow so that we can get them into practice. And we have a number of early successes with this, for example, our cardiology group has developed internally first, a novel AI based algorithm that can give you a measure of blood potassium concentration from an ECG wave form. So, from a wearable ECG monitor, you can also measure blood potassium, which has a huge impact on cardiac function. And this has now been licensed to a company that’s provided it as a wearable product. So it is on the market. And many of our groups have AI engineers now embedded into them to help in the various specialties. So, whether it be neurology or CV, cardiovascular, or even GI we’re seeing the huge power of that to really impact our care in the future.
What does the future of healthcare look like?
Well, it’s going to be amazing first of all. But I think when you think about the biggest changes we’re going to see over the next decade, I think it’s care for patients at home. I think it really has to be that virtual hospital, the remote care at home is really where we’re going. There’s already hospitals in the United States that are entirely virtual. So there’s one that I’ve been following for two or three years now, it’s called mercy virtual. And it’s in Louisiana or New Orleans. I can’t recall exactly where it is, but they’re an entirely virtual hospital. So the patients are cared for at home. They send monitoring home with them. They have health care providers that do visits when the patients need it, but they have no beds. And that really is a model for the future of health care at places like Mayo clinic.
We have a lot of patients that are not really seriously ill, but we’re still caring for them in our large healthcare system. And that’s a very expensive way to do it. And so, as we’re thinking about our plans over the next decade, where we’re understanding that we’ve got to continue to be able to provide that really complex care, that can’t move to a community hospital, that can’t move to a home system when a proton beam system costs two or three or $400 million that has to be located in a central facility, but many of the other kinds of things can be done remotely. And so that’s the direction we’re moving. So, we’re going to see the healthcare systems be much more integrated with their entire network of partners and for places like Mayo clinic and Stanford and John Hopkins Cleveland clinic, they’re going to be able to expand that reach across the world.
And that’s one of the things that I’m really excited to see is how can we start providing better care to folks all over the world, especially people that just don’t have access to it. And even if you bring that back to the United States, if you look at our rural communities the doctors there are getting older and retiring and the new younger doctors aren’t, in general, wanting to go into those spaces and many communities are being left without real kind of on-demand access to healthcare. And I think that by integrating some of these remote technologies, that’s going to be a way of solving that problem and providing this kind of care to our rural communities in the United States.
Do you have an estimate or a prediction of when we can expect to see this type of integration?
Well, we’re already doing it. Mayo has what’s called “our advanced care at home initiative”, and we are figuring out how to treat patients remotely. The pandemic has really accelerated this. Prior to the pandemic, this was our plan. This is part of our 2030 plan. We know that we’re making a big push to provide remote care for patients, but the pandemic just turned everything kind of upside down. And our remote patient visits, for example, went up by I think almost 20 times within a month. And then even now, 18 months later, we have 10 times more remote visits than we had prior to the pandemic. So, it created a step change. And the other thing it did, is it convinced people that this could work because we’re finding many of our patients prefer these remote video visits for many things. Now you can’t do that for everything, obviously, but we are already seeing that move. Mayo has partnerships with companies that are providing remote monitoring and diagnose diagnostic equipment that have businesses that have been set up around that and are starting to develop and put that infrastructure together. By the time we get to 2030, I really expect this to be a routine part of our practice. This is stuff that’s happening now.
What are the primary challenges that are facing the healthcare industry today and how are advanced technologies solving these challenges?
Well, that’s a good question. And there’s kind of a couple different takes on it. One, this remote monitoring of patients make sense, but it’s hard to do it well. And, so, there’s a lot of growing pains and figuring out how do we really get good data from these devices? We’ve got the consumer wearable devices that we’re all used to the Fitbits and stuff like that. They don’t provide medical quality data, but that’s okay because what they provide is good enough for what they’re trying to do, but as we’re moving into wanting systems that are providing diagnostics or doing therapies on people, the reliability is a lot higher. And these consumer wearable companies really aren’t familiar with working in this regulatory space, so there’s a bit of a learning curve there.
I think that’s one of the big challenges. The other really big challenge that I see is being able to get access to data, to really leverage the power of AI and machine learning. There is so much data out there. For example, we could get access to everybody’s data, we really wouldn’t have to be running clinical trials so much because the real world would be a clinical trial, right? We can get at people’s comorbidities or their pre-existing conditions. We can know what their treatment was, what their outcomes were just based on normal care when we’re treating patients. And if we could access that data, that would give us the ability to really make predictions on what care is better for what patients in what conditions. But the challenge we’ve got is getting at the data.
Patient privacy is, is a big concern. And people have different views on who owns that data and who should be able to access that data. So right now, access to data is pretty much limited to the people within your own healthcare system. So Mayo can get data from Mayo patients, right? And John Hopkins get at data from John Hopkins patients. And what we really need is to have all of that data accessible so that we can make the kind of predictions and inferences that AI makes possible, but there’s then that challenge about people’s data being available. And we see the stuff in the news, there’s always one big business or another that just got hacked and you got to change all your passwords and people don’t want that to happen to their data. So there’s a big push to try to de-identify data, which is kind of the technique that Mayo and many other companies working in this space are moving towards. But for example, your ECG wave form is just as unique as your fingerprint. So, it’s really challenging sometimes to say what does de-identified data really look like? But until we answer that question, we can’t really use these tools to answer some of the big questions about health.
Digital health is improving health care through data and technology driven practices, though. A lot of the legacy organizations still exist. How do we progress widespread digital integration?
There’s a couple of issues here. One is, adoption of EMR by a lot of healthcare systems has been pretty slow. I mentioned in my talk Mayo started creating our digital record in the 1960s. So we’ve been doing this for a long time, but many of the especially regional hospitals and smaller clinics have been really slow to move into an electronic medical record. But I just read an article a few months ago that mentioned, I think about 84% of our hospital systems now have EMR. So adoption of that is coming along fairly well. And I think we’ll see more adoption in the smaller clinics and hospitals just because it’s going to provide them with the ability to do things that they can’t do right now.
So that’s the one issue. The other is simply figuring out how to access that data and really make use of it. And, right now, what would be nice is if there was something like a patient record that could travel with you, that somebody could get your complete record, but that doesn’t help solve the problem of needing to access everybody’s data to really figure out diagnostics and therapeutics. So I think we’ll see a lot of partnerships with small health systems and small clinics that partner with a big place like a Mayo or Cleveland clinic or one of the other leaders so that they can get access to those systems and some of the insights that are coming from those big systems.
AI and machine learning are gaining steam in the medical sector due to their ability to streamline various aspects of admin and patient care delivery. Though, there are pressures to advance these technologies toward a new frontier predictive medicine, for example, AI and ML for disease forecasting. How close are we to large scale adoption of this type of technology and what are the obstacles hindering progression?
I think a lot of it is the things we’ve talked about so far. I think within the big healthcare systems we’re pretty close. What we’re doing at Mayo clinic is we’re putting together something that’s called our AI factory and what we’re trying to do is create a fairly straightforward and repeatable process that our physicians and researchers can use first to evaluate a variety of machine learning based and then to have a system for moving them relatively painlessly into the clinical workflow. So that’s part of the partnership we’ve got with Google is to try to streamline that process, because we need to be able to, in a research setting, be able to determine what algorithms are going to work, train the AI systems and test them.
But when we know that they’re working, we need to be able to quickly and efficiently move them into practice. And that’s been a big focus of ours for the last couple of years is putting that infrastructure together. I’m honestly not aware of what some of the other major health care organizations are doing, but my guess is that they’re doing the same thing that Mayo is; trying to figure out how to do this, because we know that these AI tools are going to allow us to get insights that we can’t right now. If you think about it so much of the way that we analyze wave forms, for example, ECG wave forms, it’s physicians that get so familiar with it and they see subtle distinctions and they’re making measurements and they’re able to make real great pattern recognition because the brain is an awesome pattern recognition device and they’re able to really figure out some things.
But when you start adding in say, instead of one ECG, you’ve got a 12 lead ECG, and you’re trying to look at relationships between several different of the ECG wave forms. And then you’re trying to integrate data coming from other sources too, from the electronic medical record, from the genomics history of the genomic profile of a person or their family history, you’re starting to bring in data from so many different sources that the human brain can no longer conceptualize all of it, but what we can conceptualize is how to make a tool that will give us those insights. So, we’re really good at doing that, and that’s, I think the direction that we’re moving with some of this and that’s why AI has so much potential here.
Medical technology has experienced immense disruption since the Dawn of the pandemic. Do you see a mass transition from hospital-centric care medical care to home-based virtual care in the near future?
Yeah, and we did talk about how that is the direction we’re heading for sure. And what we’re trying to do is get the more routine care taken care of at home. And this presents a kind of a particular problem too, though, because when you send somebody at home, who’s maybe got a mobility problem or something because of a surgery, but they don’t need the intense monitoring that you have in a hospital, you still have to have somebody who can help them with day-to-day activities. And that caregiver then typically ends up being a family member. That’s part of what can make home health care less expensive. You’re not only in your own environment, but you’ve also got family around to help. And as it turns out we’re recognizing that when we’re doing remote care, we’re not treating just the patient we’re treating the entire family.
And that was a real insight that I don’t think that we had anticipated when we started doing this, but it turns out the caregivers have as many, or more, questions than the patient does because they’re the ones doing things, or they see something that’s a little bit different and they don’t know what to think about it. They have to have that on-demand access to our nursing staff or our physician staff to be able to ask questions about what they’re seeing or what they should be doing. So, it’s kind of an interesting way of looking at it, when you send a patient home, you’re treating a family and that was a neat realization.